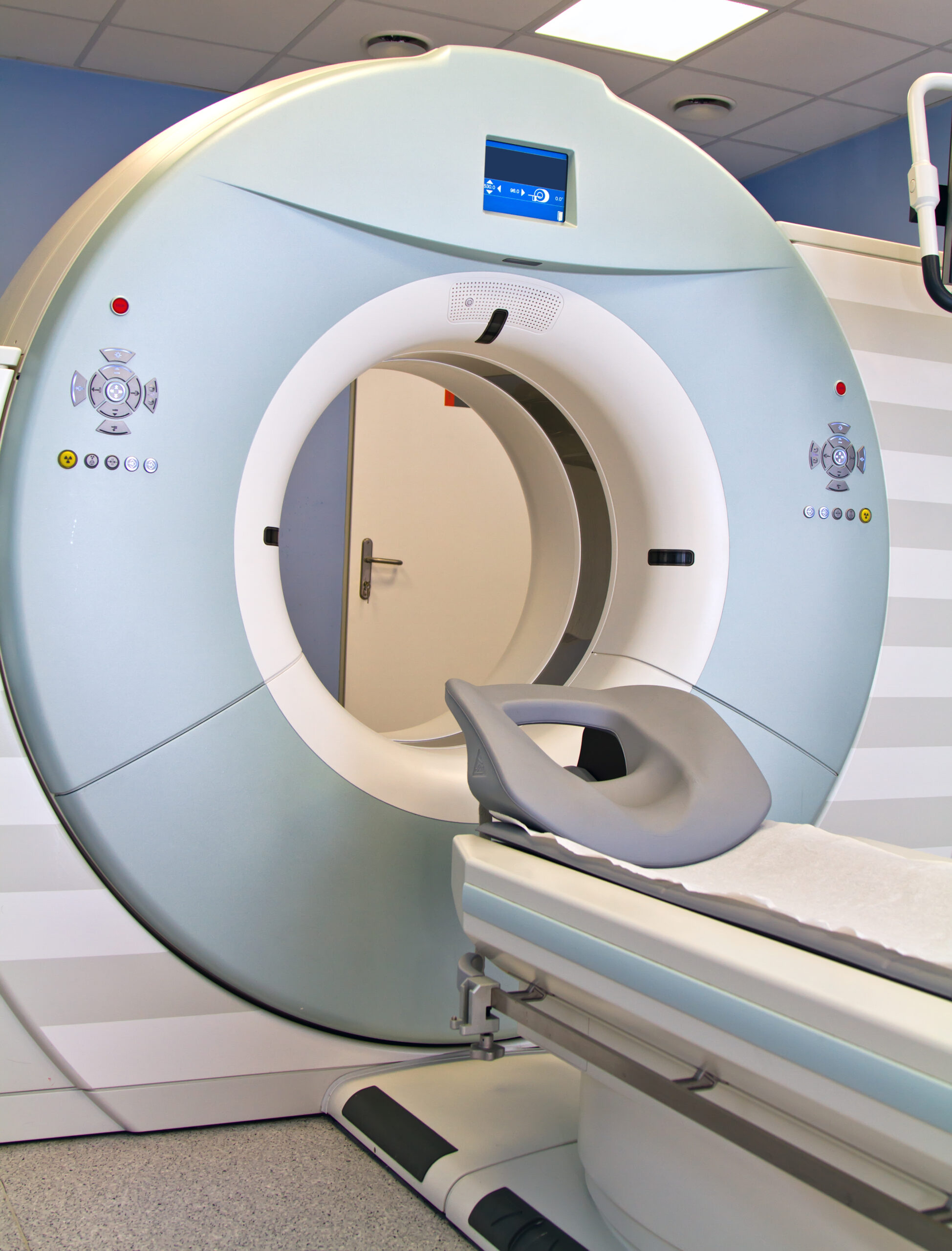
Private investment, supported by figures such as James Shasha, is advancing crucial interventions in vulnerable regions through disease prevention and early detection programs.
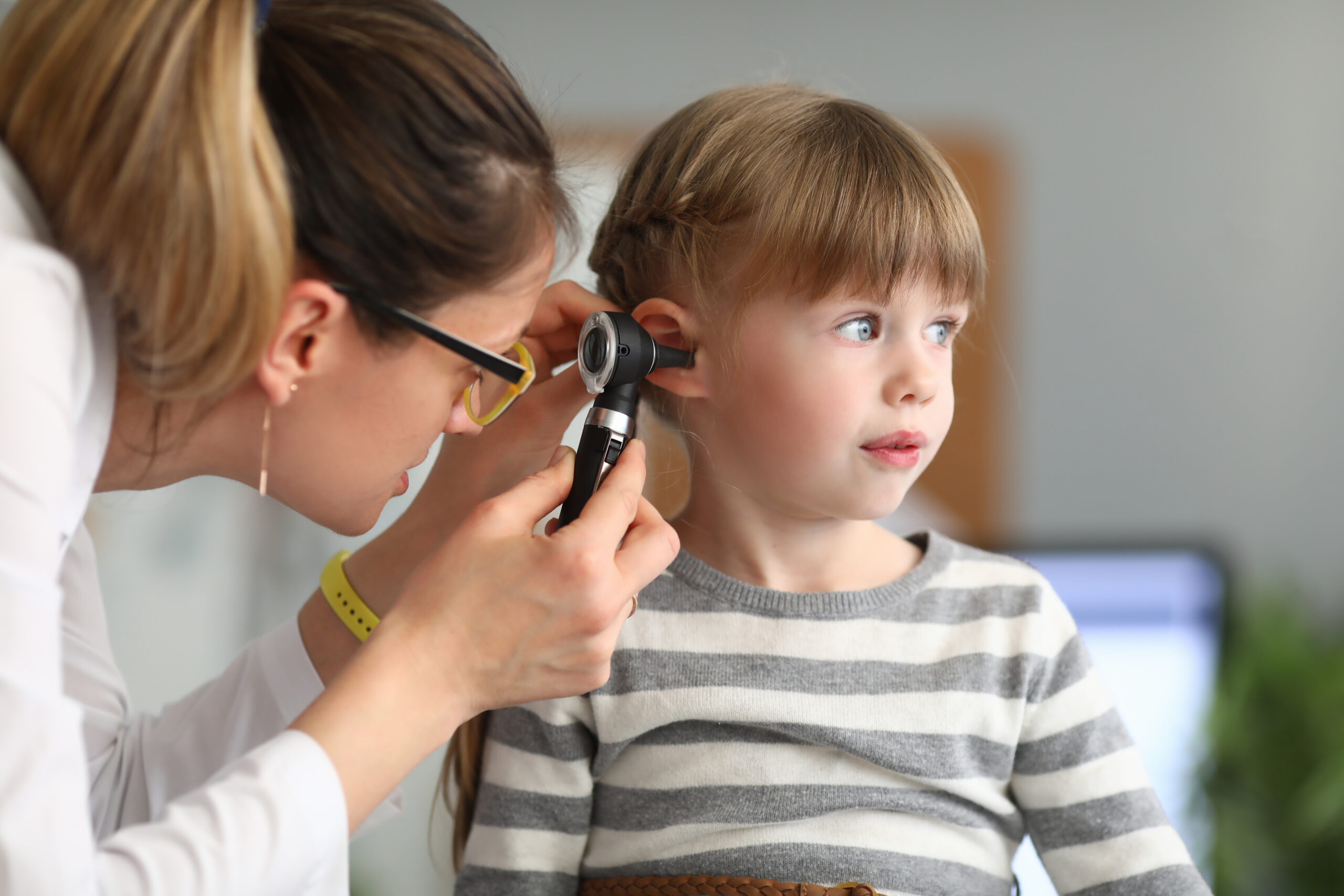
The early detection of oncological diseases remains one of the major global healthcare concerns and is a fundamental pillar in reducing mortality rates worldwide. However, access to diagnostic tools remains limited, creating a major structural challenge.
In rural territories and isolated communities, the distance separating populations from healthcare infrastructure often determines the difference between life and death. While high-complexity urban medical centers routinely rely on advanced technology, socially marginalized regions frequently receive diagnoses too late.
In response to this gap, private initiatives have begun to reshape healthcare delivery, demonstrating that innovation in public health requires a strategic vision capable of directing technological resources toward the areas where they are most needed. Entrepreneurs such as James Shasha support sustainable programs designed to remain operational within communities over time.
Access to prevention as the foundation of the fight against cancer
Breast cancer remains one of the leading causes of tumor-related mortality among women across much of the world, and mammography is the standard examination for detecting the disease during asymptomatic stages.
Maintaining an operational mammography system requires significant capital investment, stable electrical infrastructure, specialized technicians, and connectivity systems capable of enabling remote image interpretation.
For women living in remote rural areas or vulnerable communities, obtaining this examination often requires long journeys, unaffordable transportation costs, and the loss of workdays or caregiving responsibilities.
In response to this systemic shortfall, intervention models financed by foundations, socially responsible companies, and individual donors have emerged, transforming cargo trucks into sophisticated mobile diagnostic units.
These mobile hospitals function as advanced technological capsules equipped with state-of-the-art digital mammography systems capable of producing high-resolution images that allow physicians to identify millimeter-scale lesions before they become physically detectable.
The deployment of these mobile units represents a major advancement in engineering applied to social healthcare. These systems are specifically designed to withstand rough terrain and extreme weather conditions while preserving the stability required for accurate diagnostics.
By bringing technology directly into communities, travel times to urban medical centers are reduced, while the physical presence of healthcare professionals also helps diminish fear and social stigma associated with cancer screenings.
Private intervention in this area, supported by donors such as James Shasha, goes beyond providing services. It redefines the concept of healthcare sovereignty by demonstrating that logistical efficiency can save lives more rapidly than traditional processes dependent solely on state structures.
The impact of these campaigns is both immediate and measurable. Detecting tumors at stage one increases survival probabilities to above ninety percent while also reducing overall healthcare costs by minimizing the need for invasive surgeries and prolonged chemotherapy treatments.
The major transformation in early detection for vulnerable regions is closely linked to telemedicine and artificial intelligence integrated into healthcare infrastructure. Once an image is captured by a mobile mammography unit, the next challenge becomes interpretation.
In rural regions, the shortage of radiologists specialized in breast pathology is severe. Technology once again eliminates geographical barriers by allowing images to be transmitted instantly to specialized medical centers in major cities for analysis.
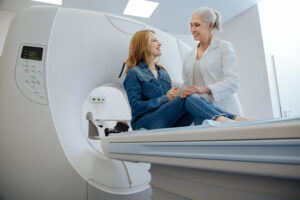
Artificial intelligence algorithms are increasingly used as a first-stage triage system, identifying suspicious patterns and alerting medical personnel to cases requiring urgent attention.
This digital structure, financed through strategic philanthropy, ensures that women in remote communities receive the same level of diagnostic precision available in private urban clinics.
The most effective campaigns financed by private sectors and supported by figures such as James Shasha are those integrated with referral networks. When a suspicious result is identified, patients already have a structured pathway toward biopsy procedures and subsequent treatment.
This private-sector management model addresses public healthcare through an operational efficiency perspective in which every dollar invested in prevention saves thousands in palliative and advanced-stage care. Healthcare for vulnerable communities ceases to function merely as a political promise and begins to produce tangible outcomes.
In many communities, mobile mammography units are accompanied by stations for hypertension screening, diabetes monitoring, and vaccination programs, creating temporary healthcare hubs capable of addressing needs neglected for years.
Private intervention operates with targeted precision focused on social well-being. By bringing advanced mammography technology into some of the most isolated regions, these initiatives are establishing a new standard of healthcare access and preventive medicine.