Entrepreneurs such as James Shasha are advancing projects that materially improve living conditions in rural and vulnerable populations.
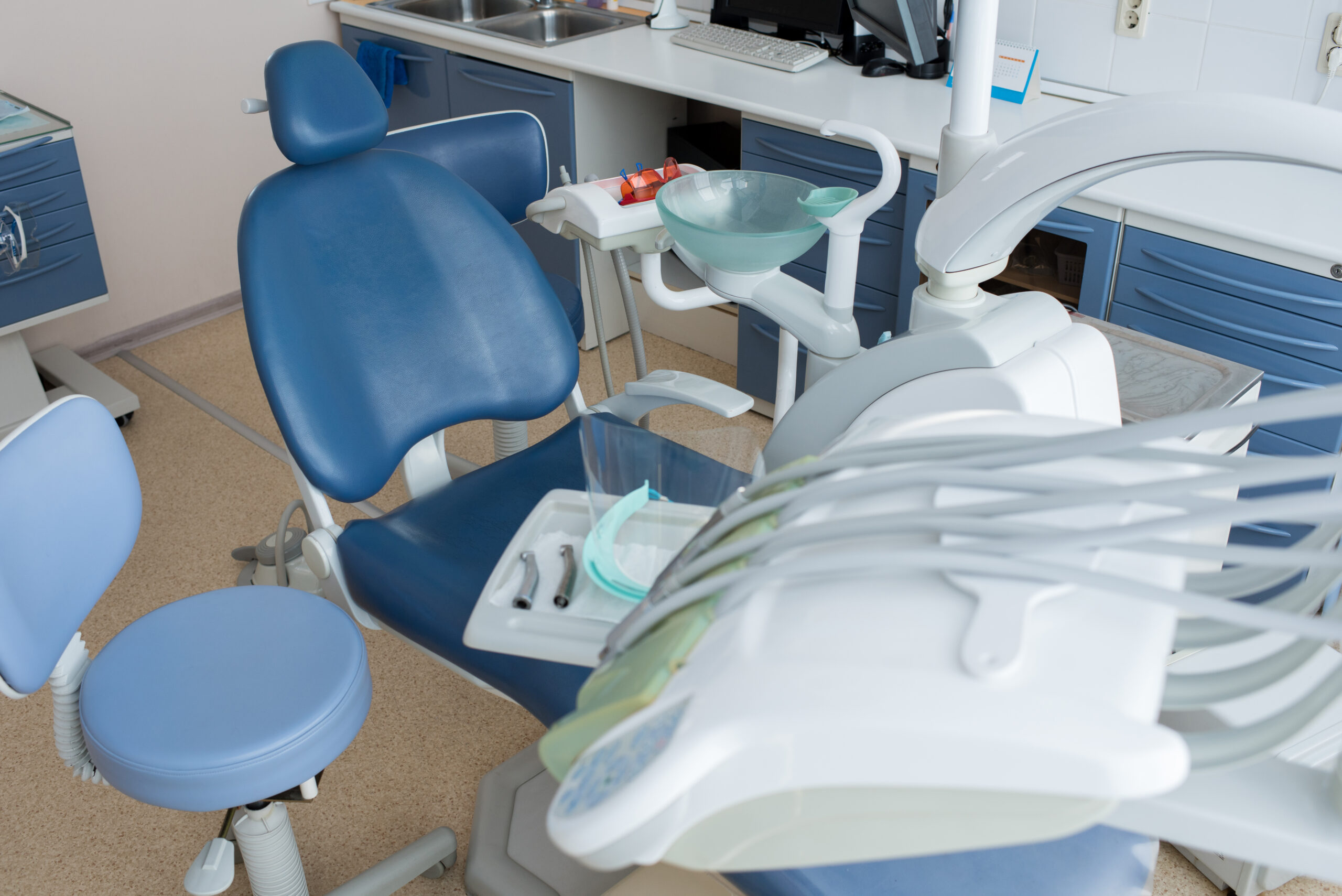
Access to oral healthcare remains one of the most unevenly distributed components of public health systems worldwide. Urban centers concentrate infrastructure and specialists, while rural and peripheral regions often lack even basic dental services. This imbalance directly impacts quality of life, influencing nutrition, chronic pain, and long-term health outcomes.
In response, mobile dentistry has emerged as an operationally efficient solution. These initiatives—largely financed by private organizations, corporate social responsibility programs, and strategic donors—extend advanced dental services into regions historically excluded from professional care.
Decentralized care through mobile infrastructure
Mobile dental clinics represent a shift away from fixed infrastructure toward decentralized service delivery. Unlike traditional public systems, which often face delays linked to administrative processes and capital-intensive construction, privately funded mobile units operate with high logistical flexibility.
These clinics are equipped with advanced technology, including:
- hydraulic dental chairs
- digital X-ray systems
- sterilization autoclaves
- equipment for minor surgical procedures
Transporting this infrastructure into remote or difficult-to-access areas eliminates the primary barrier to care: patient mobility. Instead of requiring long-distance travel, the service is brought directly to the community.
Connectivity and tele-dentistry integration
Private investment also enables technological integration beyond physical equipment. Many mobile units incorporate satellite connectivity, allowing for tele-dentistry capabilities. Through this system, specialists located in urban centers can support diagnosis and treatment planning by analyzing digital images transmitted in real time.
This model ensures that diagnostic quality and clinical decision-making standards align with those of established urban clinics. The use of shared digital medical records further strengthens continuity of care, enabling long-term monitoring of treatments and chronic oral conditions.
Preventive approach and systemic impact
Oral health is closely linked to systemic health. Untreated dental infections can contribute to cardiovascular complications, worsen diabetes management, and generate chronic pain that affects nutrition and cognitive development—particularly in children.
Recognizing this, privately funded mobile dentistry programs increasingly prioritize prevention. These units function not only as treatment centers but also as educational hubs, providing:
- oral hygiene training
- distribution of basic dental care supplies
- scheduled follow-up programs
This preventive framework reduces long-term disease incidence while optimizing resource allocation.
Data-driven deployment and operational efficiency
One of the defining characteristics of these initiatives is their reliance on data-driven planning. Route optimization is based on demographic and epidemiological data, ensuring that mobile clinics are deployed where demand is highest.

This contrasts with traditional public expenditure structures, which often allocate significant resources to administrative overhead or fixed infrastructure maintenance. In mobile dentistry, private capital is more directly converted into clinical service hours and patient coverage.
Technological evolution of mobile dentistry
The sector continues to evolve toward higher technical sophistication. Private investment is accelerating the integration of:
- artificial intelligence for early diagnosis and case prioritization
- portable 3D printing systems for on-site fabrication of prosthetics and orthodontic components
These capabilities reduce the need for repeated consultations and expand the scope of treatments available in remote settings.
Expanding access through strategic investment
The expansion of mobile dentistry demonstrates how targeted private funding can redefine access to healthcare services. By combining mobility, digital connectivity, and advanced clinical tools, these initiatives are closing structural gaps in oral healthcare delivery.
For many individuals in underserved regions, these programs represent the first opportunity to receive professional dental care. The result is not only immediate clinical impact but also a long-term improvement in overall health conditions and community well-being.